Summer may be BBQ season, but it’s also the time when people travel long distances in planes, trains, and automobiles. For us in vein healthcare, that means increased risks of Deep Vein Thombosis, or DVT.
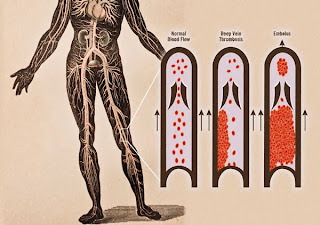
The deep vein system carries about 80% of blood from the feet back up to the heart. Deep veins are located under the muscle and connective tissue layers in the legs. A blood clot in a deep vein can be dangerous because the high pressure in the system could cause the clot to break free from the vein wall and enter the blood stream. The DVT could then travel up through the legs into another part of the body such as the lungs, where it would become a pulmonary embolism (PE).DVT or PE symptoms are often misinterpreted as something less serious. A blood clot in the leg may feel like a “charley horse,” shin splints, or a twisted ankle. Symptoms from PE are often attributed to a pulled muscle in the chest, costochondritis (inflammation of the joint between ribs and breast bone), asthma, or a “touch of pneumonia.”
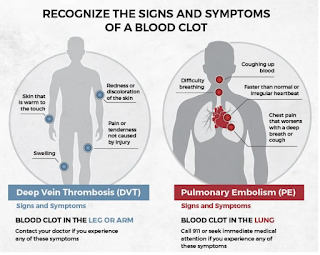
So what are some of the signs to look for? For DVT, the leg may be warm to the touch; swelling in the leg (can also occur in the arm); leg (or arm) pain or tenderness; reddish or bluish skin discoloration.
For PE, be aware of a sudden shortness of breath; sharp, stabbing chest pain (may get worse with deep breath); rapid heart rate or breathing; feeling lightheaded or fainting; unexplained coughing, sometimes with bloody mucus.
In half of DVT and PE cases, no symptoms present at all—but both conditions are medical emergencies. Any of these symptoms should be regarded as a DVT or PE until proven otherwise, especially if someone is in a risk category (including whether there is a history of blood clots in your family).
Awareness is key-- and so is prevention. When traveling long distances, stay well hydrated, stretch legs your legs and pump your feet periodically, avoid or moderate alcohol and caffeine, and consider wearing graduated compression stockings on your trip.
To find out more about DVT and other vein issues, contact us at the Vein Healthcare Center. We will evaluate your vein health — including spider veins, varicose veins, and leg ulcers.